SAMHSA to Update Federal Rules to Expand Access to Opioid Treatment
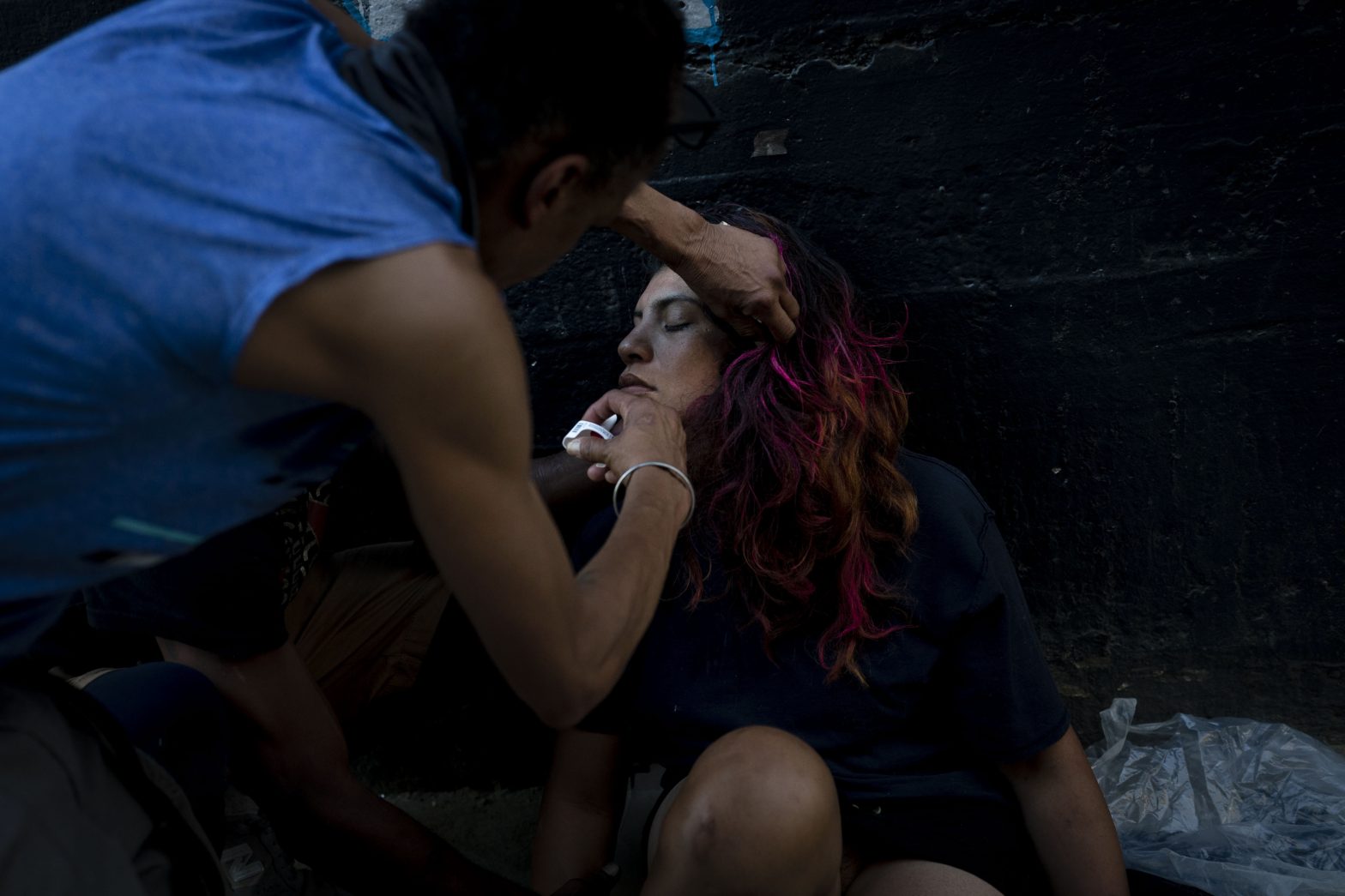
The Substance Abuse and Mental Health Services Administration is seeking to update federal regulations that govern opioid use disorder treatment to allow those struggling with addiction to take home doses of methadone and use telehealth to initiate buprenorphine at opioid treatment programs.
According to the Centers for Disease Control and Prevention, more than 107,000 Americans died from drug overdoses in 2021, an increase of more than 15% from 2020.
The agency believes the changes it is proposing to 42 CFR Part 8 could help reduce overdose deaths.
“These proposed updates would address longstanding barriers to treatment in regulations — most of which have not been revised in more than 20 years,” said Miriam Delphin-Rittmon, the HHS assistant secretary for Mental Health and Substance Use and the leader of SAMHSA, in a written statement.
“I am committed to moving these forward as quickly as possible because we have heard from both providers and patients how urgent the need is for treatment,” she said.
SAMHSA specifically proposes to update Part 8 by removing stigmatizing or outdated language; supporting a more patient-centered approach; and reducing barriers to receiving care.
For example, in March and April 2020, SAMHSA published flexibilities for the provision of take-home doses of methadone and for the use of telehealth in initiating buprenorphine in opioid treatment programs.
Patients deemed stable by physicians have been able to take home up to 28 days’ worth of methadone doses; other patients — again, so determined by their physicians — received up to a 14-day supply.
A recent study showed that patients who received increased take-home doses after federal flexibilities were enacted during COVID-19 saw positive impacts on their recovery, including being more likely to remain in treatment and less likely to use illicit opioids.
These flexibilities represented the first substantial change to opioid treatment standards in more than 20 years. Under the Notice of Proposed Rulemaking for Part 8, SAMHSA proposes to make these flexibilities permanent.
SAMHSA’s proposed changes also would update standards to reflect an Opioid Treatment Program accreditation and treatment environment that has evolved since Part 8 went into effect in 2001.
Accordingly, SAMHSA proposes updates that reflect evidence-based practice, language that aligns with current medical terminology, effective patient engagement approaches and the workforce providing services in opioid treatment programs, including:
- Expanding the definition of an opioid treatment program treatment practitioner to include any provider who is appropriately licensed to dispense and/or prescribe approved medications.
- Adding evidence-based delivery models of care such as split dosing, telehealth and harm-reduction activities.
- Removing such outdated terms as “detoxification.”
- Updating criteria for provision of take-home doses of methadone.
- Strengthening the patient-practitioner relationship through promotion of shared and evidence-based decision-making.
- Allowing for early access to take-home doses of methadone for all patients, to promote flexibility in creation of plans of care that facilitate such everyday needs as employment, while also affording people with unstable access to reliable transportation the opportunity to also receive treatment; likewise, promoting mobile medication units to expand an opioid treatment program’s geographic reach.
- Reviewing opioid treatment program accreditation standards.
To facilitate expansion of access to care, SAMHSA proposes to update opioid treatment program admission criteria in Part 8.
This includes removal of the one-year requirement for opioid addiction before admission to an opioid treatment program, in favor of considering a person’s problematic patterns of opioid use. In conjunction with updated standards that include extended take-home doses of methadone and access to telehealth, these changes are likely to expand access while also improving retention in treatment.
The Notice of Proposed Rulemaking also proposes to eliminate the requirement that practitioners who have a waiver to prescribe buprenorphine for up to 275 patients provide reports to SAMHSA on an annual basis.
The Notice of Proposed Rulemaking also promotes the chronic disease model of management, while removing barriers to providing individualized care.
“Removing these barriers promotes patient trust and reduces the need for individuals to attend an opioid treatment program each day to receive treatment services,” said Assistant Secretary Delphin-Rittmon. “In this way, the proposed changes to Part 8 are focused on the individual and their treatment environment.”























