Digestive Health Is Women’s Health. Insurance Barriers Block Access to Both.
COMMENTARY
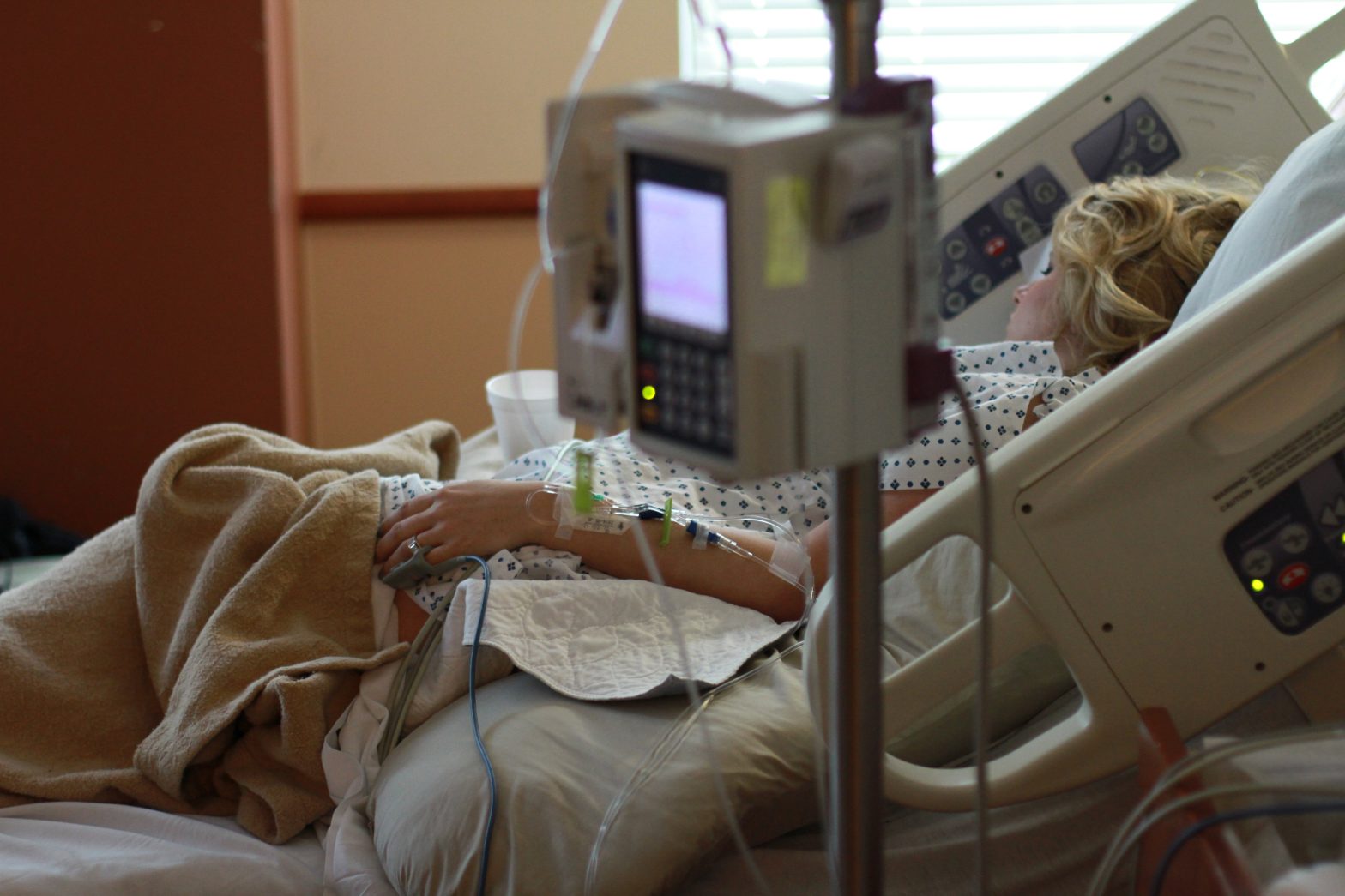
All too often, our nation’s health care system dismisses women and their health concerns. Women feel discounted by their doctors when sharing their health histories or feel unfairly exploited by insurance company barriers when treatments are delayed or denied.
These experiences raise concerns about access to care and have serious implications on women’s health if they cannot get timely diagnoses or treatments.
As a gastroenterologist here in Philadelphia, Pennsylvania, I hear how concerned my female patients are during every clinic session.
Women are particularly vulnerable to digestive issues, which inspires me to advance health equity in a field that few people associate with women’s health.
In order to address the significant barriers to care that many women face, the Penn Women’s FIRST Clinic was founded. It provides unique, multidisciplinary care for women. But, despite such efforts, even when a doctor determines the type of gastrointestinal care a woman needs, she is often prevented from accessing it due to insurance barriers.
If insurance companies are serious about women’s health, they need to reevaluate — or reverse — policies that make it harder for women to access treatments, such as prior authorization.
Prior authorization is an all-too-common insurance barrier that prevents patients from getting the care they need when they need it. It requires doctors to get approval from the health insurance company before giving a patient a prescribed treatment or procedure.
Insurance companies say this is to prevent unnecessary care, but really, they are trying to limit their costs.
Frustratingly, prior authorization happens all the time: 94% of doctors say they have patients impacted by the practice, 80% say this sometimes leads to treatment abandonment and 25% say prior authorization has led to a patient being hospitalized.
This is a widespread problem across medicine — including gastroenterology and women’s health. Consider the following examples.
When undergoing fertility treatments or experiencing pregnancy, the hormonal and physical changes that occur as a fetus develops often lead to serious constipation. My first course of prescribed treatment is to provide over-the-counter laxatives, but when they are ineffective, we have to try specialty treatments.
Despite how common this experience is for women, prior authorization is incredibly prevalent, forcing women to wait for their insurers to scrutinize prescriptions, double-check paperwork, handle appeals and sometimes meet with doctors for peer reviews before (hopefully) approving the drugs these women should have gotten without delay.
Delays in this process result in intense discomfort, psychological distress and disruptions to patients’ daily lives.
Another worrying example is UnitedHealthcare’s recent push to implement a “Gold Card” prior authorization program that would require insurance approval for virtually all endoscopies and colonoscopies that its 27 million commercial beneficiaries need. These procedures are absolutely critical for diagnosing and surveilling diseases such as inflammatory bowel disease and colorectal cancer — the second deadliest cancer in the United States.
Right now, the insurer is building the groundwork for prior authorization in “early 2024.” If UHC pushes forward with prior authorization for these critical procedures, the results will be disastrous for patients.
For pregnant women in particular, delays in endoscopy can have significant consequences: Typically endoscopy is scheduled to occur during the second trimester as this is considered the safest time frame and we only perform procedures in pregnancy when they are absolutely necessary. However, with pending prior authorization requirements from UHC, patients would face delays and further challenges to schedule within this critical window, potentially leading to harm to both the mother and the baby.
Barriers to care don’t stop there: Insurers are also increasingly invoking step therapy or “fail first” policies that impact care for patients with IBD.
Step therapy occurs when a GI prescribes a biologic therapy for an IBD patient who is usually very sick with a flare, but the insurance company denies coverage. Instead, the insurer forces the patient to “step” through more basic/less costly therapies and fail before being able to get the more effective and costly biologic their doctor prescribed.
According to one study, nearly half of patients who need biologics or immunologic drugs are forced to try one or more therapies with safety warnings before they can access a safer treatment. All too often, women are in the crosshairs of these frustrating barriers.
At the end of the day, processes like prior authorization and step therapy show how insurers only give lip service to health equity but make it harder for patients to access lifesaving treatments.
Insurers must be held accountable for policies that could potentially harm millions of patients.
Shazia Siddique, MD, MSHP, is the chair-elect of the American Gastroenterological Association’s Government Affairs Committee. Siddique can be reached at gastro.org.
























