CDC Revises Guidelines for Using Opioids to Treat Pain
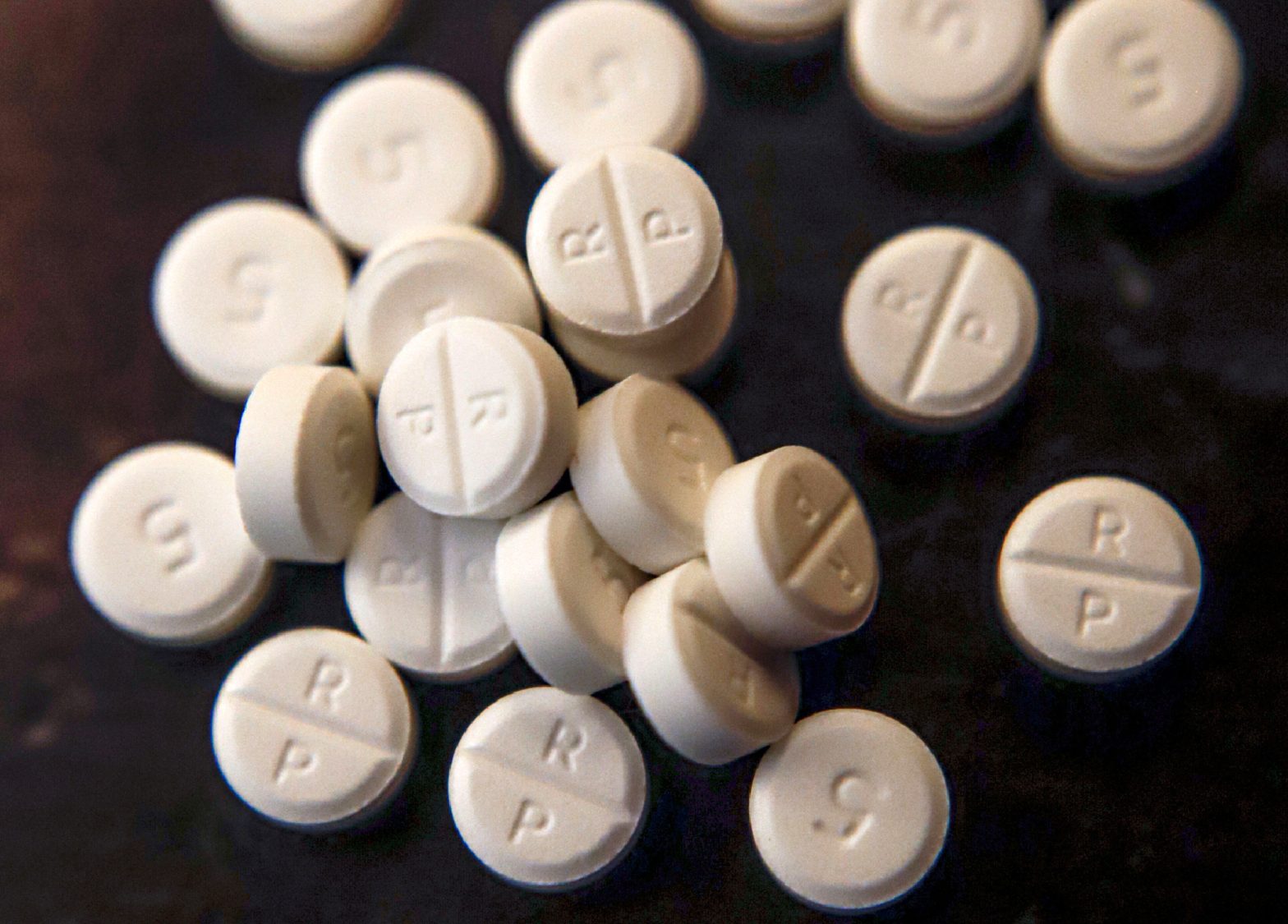
ATLANTA — The Centers for Disease Control and Prevention has revised its guidelines for using opioids to treat pain, removing dose and duration targets due to unintended consequences stemming from its earlier recommendations.
The new guidance, announced Thursday, updated advice issued in 2016 that was in part a response to the overprescribing that led to the nation’s opioid overdose epidemic.
Almost from the moment the old recommendations were released, however, critics panned the directive, saying they focused on addressing one serious problem while creating a number of new ones, including causing some long-term pain sufferers to be cut off from the medication that was their only source of relief.
In a commentary published in Thursday’s New England Journal of Medicine, the authors of the guidelines said their work in 2016 was associated with “accelerated reductions in overall and potentially high-risk prescribing of opioids and with increases in prescribing of nonopioid pain medications.”
But, they added, “new laws, regulations, and policies, in some cases purportedly derived from the 2016 guideline, went beyond — and were inconsistent with — its recommendations.”
“Such misapplication, including inflexible application of recommended dosage and duration thresholds, contributed to patient harms, including untreated and undertreated pain, rapid opioid tapers and abrupt discontinuations, acute withdrawal symptoms, and psychological distress, in some cases leading to suicidal ideation and behavior,” they said.
The new guidelines were reviewed by an independent federal advisory committee, four peer reviewers and members of the general public.
The CDC then reviewed the feedback it received and revised the authors’ draft guidelines to reflect appropriate changes.
Overall, the new guidance stresses the need for individualized care when it comes to pain management.
It also emphasized four key points, the authors said, namely, that “there are persistent barriers to access to pain care and evidence-based treatment; shared decision making by patients and clinicians is critical; discontinuing opioids after extended use can be very challenging and potentially harmful, especially if doses are tapered rapidly or patients do not receive effective support; and the new recommendations need to be communicated and implemented carefully.”
As a result, the new guidelines no longer advise doctors to avoid increasing dosages to 90 morphine milligram equivalents or more per day.
Such equivalents are defined as the amount of milligrams of morphine an opioid dose is equal to when prescribed.
As of Thursday the guidelines merely say that “clinicians should prescribe the lowest effective dosage.”
The original guidance also said that when it came to acute pain, prescriptions lasting “three days or less will often be sufficient; more than seven days will rarely be needed.”
The problem was some doctors and many policymakers took that recommendation to represent a hard stop, leading many chronic pain sufferers to seek illicit sources of relief when their prescriptions were overly tapered.
“New guidance informed by emerging data advises clinicians to carefully weigh benefits and risks of tapering opioids along with benefits and risks of continuing opioids and emphasizes that opioid therapy should generally not be discontinued abruptly, nor should doses be reduced rapidly,” the authors wrote in their NEJM commentary.
“When patients have been taking opioids for longer durations (e.g., ≥ 1 year), dosages that are tapered by 10% per month or slower will most likely be better tolerated than more rapid tapers,” they wrote.
“Although clinicians and patients might not always be able to agree on whether tapering is necessary, the guideline describes an approach to implementing treatment changes in a patient-centered manner, while avoiding abandoning the patient and instead drawing on clinicians’ empathy and principles of shared decision making,” they added.
The CDC said Thursday that it will continue to monitor the new guidelines for both intended and unintended effects and will work with the public and insurers “to inform decisions regarding coverage of a broader range of pain therapies.”
The authors — Deborah Dowell, M.D., M.P.H., Kathleen R. Ragan, M.S.P.H., Christopher M. Jones, Pharm.D., Dr.P.H., Grant T. Baldwin, Ph.D., M.P.H., and Roger Chou, M.D. — stressed in their commentary that evidence to guide the best achievable pain management remains limited.
“Research should address critical remaining gaps, including long-term comparative effectiveness of therapies for pain,” they wrote, adding that “patient–clinician communication about benefits and risks associated with opioids remains central to treatment decisions.”
Dan can be reached at [email protected] and @DanMcCue

























