We Have the Tools to Address Opioid Addiction at its Core, But Do We Have the Political Will to Take Action?
COMMENTARY
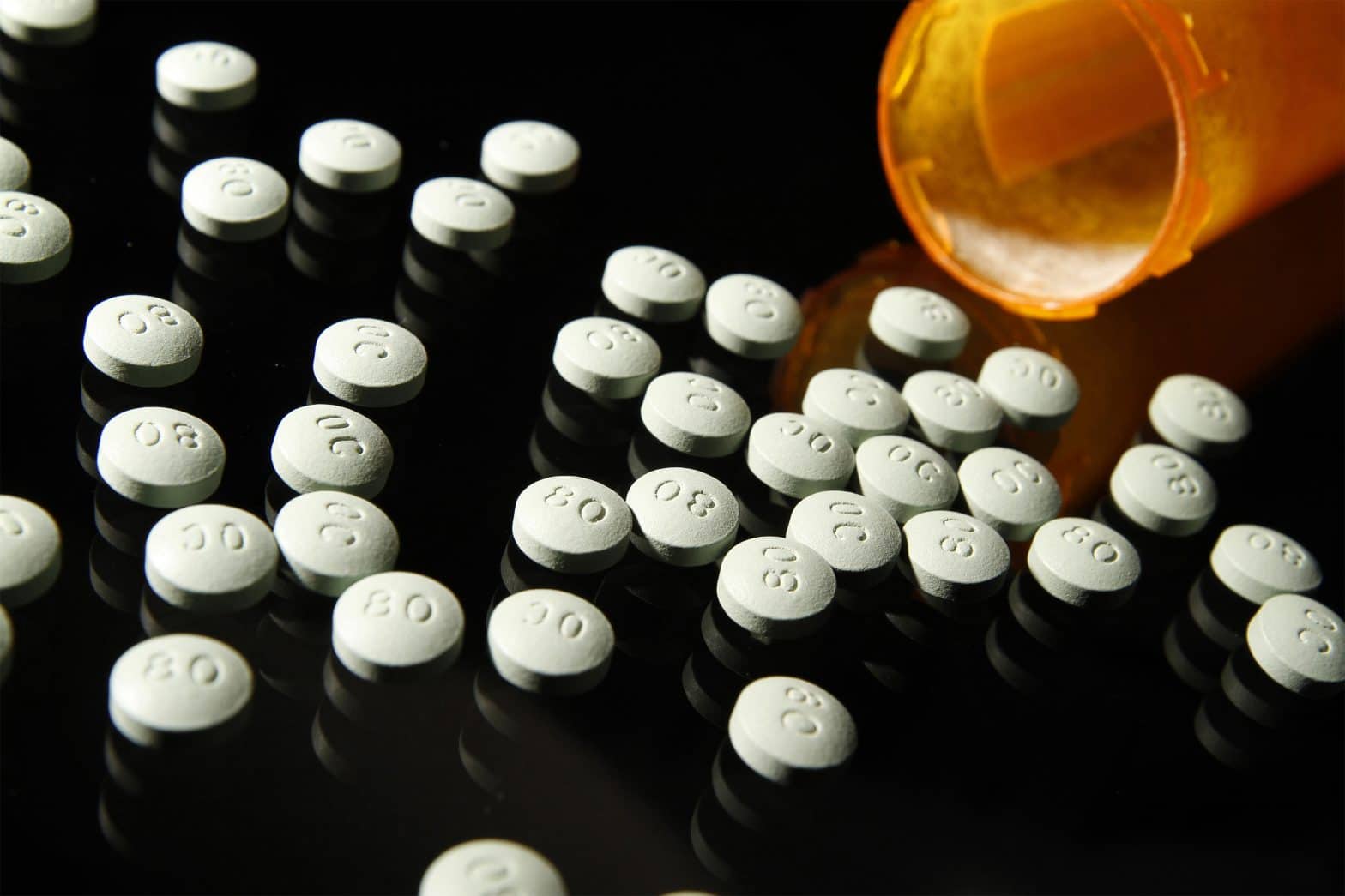
Having recently finished the original docuseries “Dopesick,” it occurred to me that many Americans may just be learning how opioid abuse turned thousands of patients into addicts and then into inmates.
As the CEO of one of the nation’s largest correctional health care providers, I have witnessed the toll of opioids on many otherwise law-abiding Americans — because they end up in our care.
The country now has an opportunity to break the tragic cycle between opioid use, addiction and incarceration. With a $6 billion settlement offer from the founders of Purdue Pharma, $26 billion from other manufacturers and distributors, and the billions of dollars yet to be collected, policymakers must aggressively rethink addiction care at one of the last stops for addicts — prisons and jails.
This will require our leaders to step up and reverse decades of underfunding for inmate behavioral health, as well as embracing evidence-based models of treatment.
The opioid story begins with large pharmaceutical companies’ targeted and deceitful marketing to poor suburban and rural communities to drive sales for the strongest versions of addictive OxyContin to the highest-volume prescribers.
For decades, a shockingly large part of our country’s health care infrastructure fed cycles of addiction, misery and death. The number of Americans arrested for drug possession has tripled since 1980, alongside the rise in opioid use. Overdose deaths in the United States now top 100,000 per year and are rising fastest amongst Black men. Fatal overdoses rose by more than 40% in Washington, D.C., and Virginia in the last year — a climb that continues across the country.
The opioid epidemic is estimated to cost our economy at least $1.3 trillion annually. Compare that to the meager billions in settlements with drug manufacturers and distributors.
No population has been as disproportionately harmed by the opioid crisis as the presently and formerly incarcerated.
At least 25% of those with Opioid Use Disorder have had an encounter with the criminal justice system in the past year. And as the severity of disorder increases, so does the likelihood and magnitude of involvement with the criminal justice system.
Among our patient population at Corizon, soon to be YesCare, close to half battle drug dependence. In Maryland, 70% of individuals suffer from substance abuse or dependence upon entering the system, and there, as is the case nationally, opioid overdoses are the leading cause of death upon re-entry to their communities. However, there is considerable evidence that Medication-Assisted Treatment during and after incarceration breaks the vicious cycle of relapse and recidivism.
Addiction often is seen as a criminal choice, rather than a disease in need of treatment.
Our patients often come from communities that lack robust and well-funded systems of care for behavioral and mental health. Without other support, many people turn to self-medication. Ultimately, they land in our care at various entry points of the criminal justice system, which is the first time many of them receive any sort of treatment at all.
Having seen the connection between incarceration and addiction up close, I can attest to the critical importance of treating addiction in correctional settings as a public health issue.
We must apply the settlement monies by thoughtfully using evidence-based practices that free people from cycles of addiction, which benefits not only them, but also their loved ones and communities. Reflecting the impact of the opioid crisis, a disproportionate share of these funds should be invested in addiction treatment, including MAT, in state and county prison systems nationwide.
Our patients are disproportionately victims of the opioid epidemic and deserve treatment that will increase their chances for success upon release — a win-win for all, given that 95% of formerly incarcerated individuals return to their communities. We will not solve the opioid crisis until we break the connection between incarceration and addiction.
My fear is that this is not the popular choice, nor the choice that polls well, but investing in addiction treatment as an integral part of correctional health programs is the right and fiscally sound choice.
Society continues to pay the price — in lives lost and ruined, in communities ravaged by crime — for our shortsighted embrace of this “magic pill.” My company is determined to do its part by helping those in our care devastated by opioids return safely to their communities. We intend to lead by partnering with state and local governments to fight for and guide spending of settlement dollars so that their communities receive the highest return on investment.
By shepherding funds from opioid settlements toward treating opioid use disorder among the incarcerated, we can address the problem at its core. By breaking the addiction-to-prison pipeline, we can save productive lives, make our communities safer and make progress toward finally ending the opioid tragedy.
Sara Tirschwell is the chief executive officer of Corizon, soon to be YesCare. For four years she was the chief financial officer of Foundation House, an addiction treatment center in Portland, Maine. With more than 30 years of experience in distressed finance, she has been intimately involved with numerous settlements of similar mass-tort litigations. You can reach Sara by email, LinkedIn, or Twitter @STirschwell.























