Protecting Our Health Care Heroes
COMMENTARY
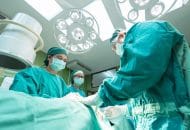
At the height of the first COVID-19 wave, hospitals tried their best to protect health care workers, but it wasn’t enough. Nearly 4,000 U.S. health care workers died during that first wave from being exposed. As the number of patients dependent on ventilators and high flow systems dramatically increased, there was a dire need to provide critical patients with life support therapy. While states struggled to find enough ventilators and high flow systems to meet the demand, hospital staff nationwide struggled to find access to the critical personal protective equipment they needed to protect their lives while saving others. Over a year later as delta variant cases surge – with lambda variants right behind them – similar concerns are resurfacing.
From the outside looking in, it seemed obvious to prioritize the equipment needed to keep patients alive. But from the inside, as a respiratory therapist, I’ve witnessed in real-time the devastating toll this pandemic has taken and continues to take on our health care heroes. While it’s important to treat as many patients as possible, what happens when health care workers are left unprotected? When we think about protecting the front-line of defense in our health care system, we should also be thinking about how we can best protect the individuals risking their lives to save others, especially in a public health crisis. In the case of COVID-19, U.S. health care workers were left without adequate protection, and that should never happen again.
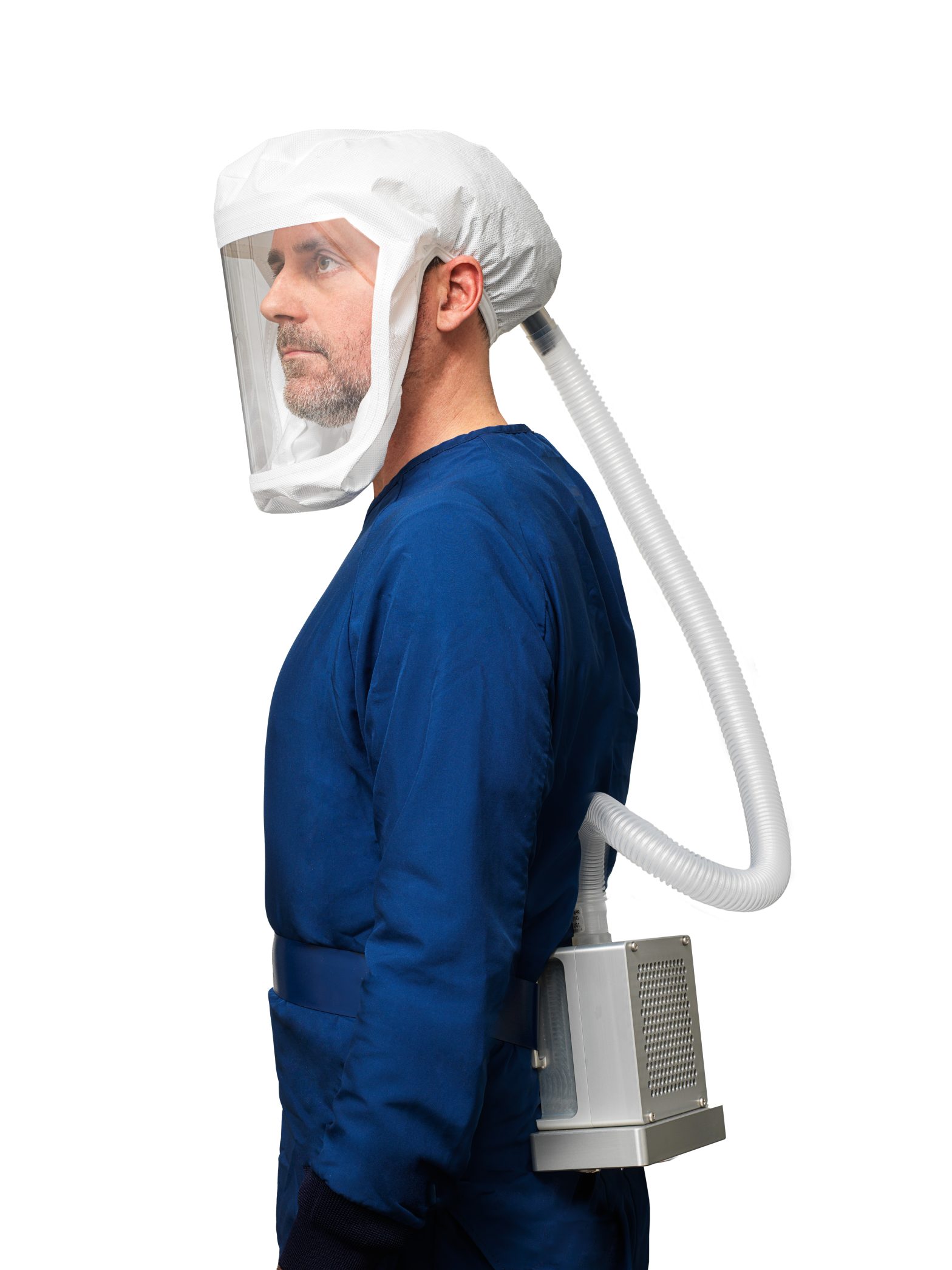
When the pandemic began, supplies were being shipped across the globe. Countries all over the world were overwhelmed and rushing to get equipment, including America. While face masks and consumable N95s are helpful for patients and limited one-time use, they’re not as durable and effective for medical professionals working non-stop. Consumable N95s and surgical masks are important, but they’re not built to withstand the daily wear and tear when treating patients during a pandemic like COVID-19. PPE that allows health care workers to spend long periods of time in rooms with patients, such as powered air-purifying respirators or face shields were what health care workers really needed.
Yet, like surgical face masks and N95s, the amount of PAPRs and required filters available were few and far between, leaving hospitals to settle for masks that are less-effective, less-comfortable, and over time — more expensive. We saw colleagues with scarring from having to wear multiple face masks or N95s over excruciatingly long periods of time. Communication barriers increased because mouths could not be seen, whereas PAPR hoods or facial shields with clear coverings allow for easier communication between the patient and the health care worker.
While many small business manufacturers in the United States have been eager to play a larger role in producing PPE, including PAPRs, they’ve been met with challenges in competing with larger contractors who rely on foreign manufacturing, often at the expense of standards. The pandemic has made it clear there is a cost to reliance on low-cost manufacturing in China.
Many of my colleagues have experienced these costs directly. Importing PPE from China increased shipping costs, delayed shipping times and most importantly, put lives at stake through faulty equipment. While the immediate concern was a shortage of respirators for patients, health care workers suffered from the lack of protection, and many paid the ultimate price. As delta variant cases take hold in China, some of their factories have shut down and the limited PPE available is being used to support their own crisis.
We must learn from the first wave and do our best to prevent any version of these challenges from occurring again. The reintroduced U.S. Innovation and Competition Act, which includes the proposed Make PPE in America Act along with the president’s executive order to revamp the Strategic National Stockpile, are both crucial steps for the future of our health care system. It acknowledges the significant vulnerabilities in our supply chain and incentivizes the domestic manufacturing and purchasing of PPE. Not only does this help to protect our health care system, it re-shores jobs and manufacturing, promoting America’s global competitiveness and ensuring broader access to quality equipment.
These benefits reach far beyond our health care industry. By incentivizing the domestic manufacturing of PAPRs and other PPE, Congress can also help protect industrial workers, firefighters, and other first responders. From Florida to Washington, we’ve seen recently how unpredictable the need for specialized equipment can be. Especially in times like these, it is crucial to have access to authentic, up-to-standard PPE. This is precisely why we cannot continue to rely on unreliable partners.
America’s manufacturing resources are vast, but we need policies that enable them, not handicap them at the expense of our critical health care workers. With the smart incentives the Make PPE in America establishes, we can help safeguard America’s health care system from our supply chain to our health care workers and ultimately, to every patient.
Felix Khusid, RRT-ACCS, NPS, RPFT, FAARC, FCCM, FCCP, ATSF, is the president of the New York Downstate Association for Respiratory Therapists. Khusid was awarded as a 2020 Respiratory Acute Care Practitioner by the American Association for Respiratory Care. His research and expertise include the Application of Advanced Ventilatory Modalities, High Frequency Percussive Ventilation and Ventilator Graphics Analysis. Khusid is also the former co-director for Mechanical Ventilation Workshops conducted by the American College of Physicians.