A Probiotic May Control Serious Antibiotic-Resistant Staph Infection
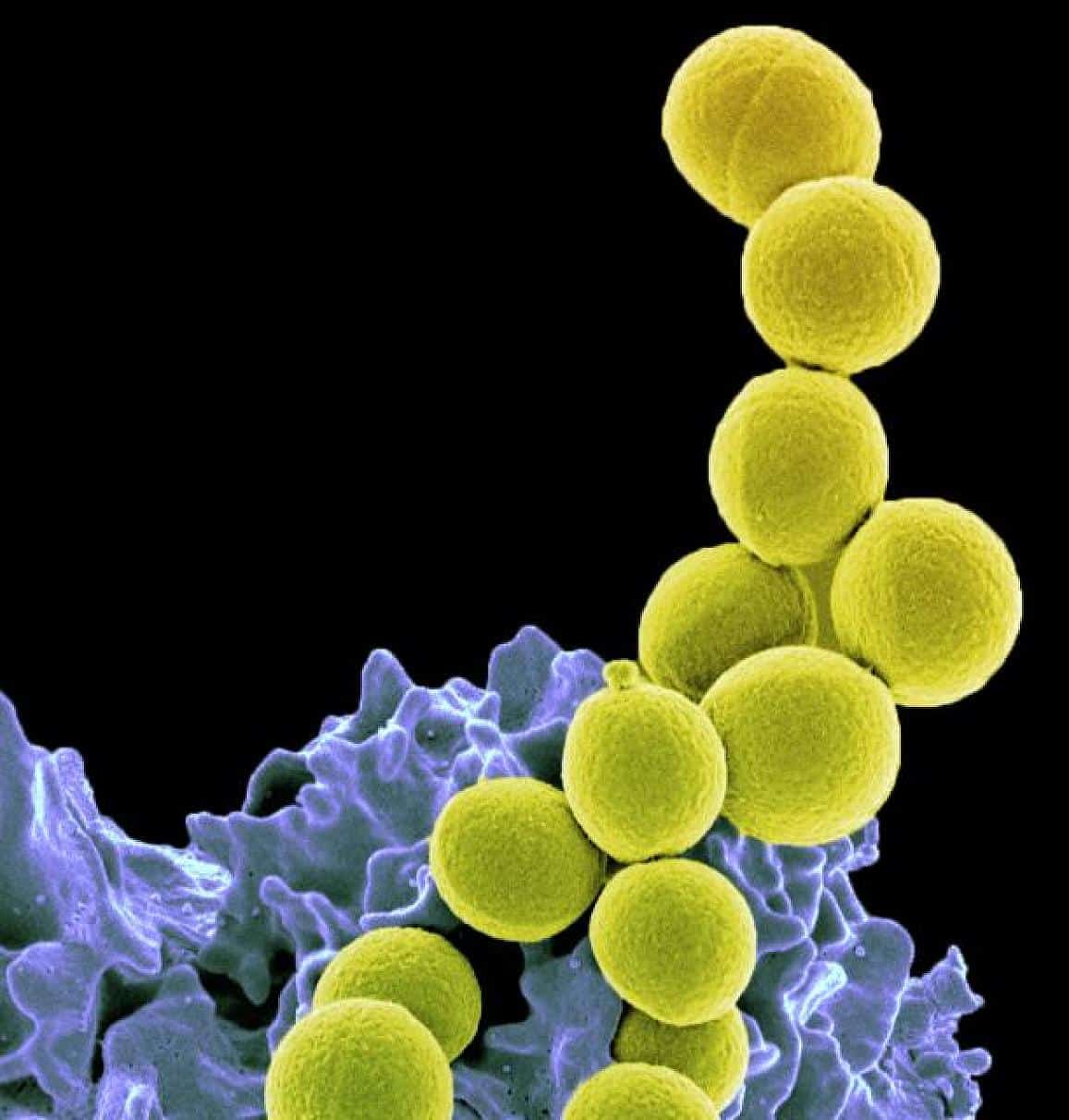
WASHINGTON — A probiotic may be effective in cleansing the body of staph-related super infections, according to a new study from the National Institute of Allergy and Infectious Diseases.
Though they say more research is needed, a press release on the institute’s website stated that their initial findings could lead to a way to prevent Staphylococcus aureus infections.
Their work was published in The Lancet Microbe.
Staphylococcus aureus, also known as S. aureus, typically causes skin infections and can lead to potentially fatal diseases if it gets into the bloodstream.
Infections caused by this pathogen are common in community-acquired and hospital-acquired settings, but treatment is challenging due to the prevalence of drug resistant strains.
The new study, conducted by researchers led by Michael Otto, Ph.D., an NIH senior investigator at the National Institute of Allergy and Infectious Diseases, found that the probiotic Bacillus subtilis markedly reduced S. aureus colonization in trial participants without harming the gut microbiota, which includes bacteria that can benefit people.
Methicillin-resistant S. aureus, or MRSA, is familiar to many people as a cause of serious disease.
Less well known is that S. aureus often lives in the nose, on the body and in the gut without causing any harm. However, if the skin barrier is broken, or the immune system compromised, these colonizing bacteria can cause serious skin, bone, lung and blood infections.
The prevention of S. aureus infections using approaches to “decolonize” the body has gained increased attention as the spread of antibiotic resistance limits treatment options, a press release from the institute said.
Some decolonization strategies are controversial because they also require large amounts of antibiotics, raising concerns about damage to the microbiota and the development of antibiotic resistance.
So far, it appears that only nasal S. aureus colonization can be targeted with topical antibiotics without doing too much harm, but bacteria quickly can recolonize in the nose from the gut.
Probiotics, digestive supplements containing live microorganisms, may be a way to complement or replace antibiotics.
Probiotic bacillus is especially promising because it is administered orally as spores that can survive passage through the stomach and then temporarily grow in the intestine.
In prior studies, Otto’s group discovered an S. aureus sensing system needed for S. aureus to grow in the gut.
They also found that fengycins, bacillus lipopeptides that are part peptide and part lipid, prevent the S. aureus sensing system from functioning, thereby eliminating the bacteria.
In the clinical trial, the research team tested 115 healthy participants, all of whom were colonized naturally with S. aureus. A group of 55 people received B. subtilis probiotic once daily for four weeks; a control group of 60 people received a placebo.
After four weeks researchers evaluated the participants’ S. aureus levels in the gut and nose. They found no changes in the control group, but in the probiotic group they observed a 96.8% S. aureus reduction in the stool and a 65.4% reduction in the nose.
Otto has emphasized in interviews that the probiotic used in the research did not kill S. aureus, but it strongly diminished its capacity to colonize.
The researchers plan to continue their work by testing the probiotic in a larger and longer trial. They note that their approach probably does not work as quickly as antibiotics, but can be used for long periods because the probiotic as used in the clinical trial does not cause harm.
Study collaborators in Thailand are from Rajamangala University of Technology Srivijaya, and Prince of Songkla University.
Dan can be reached at [email protected] and at https://twitter.com/DanMcCue

























